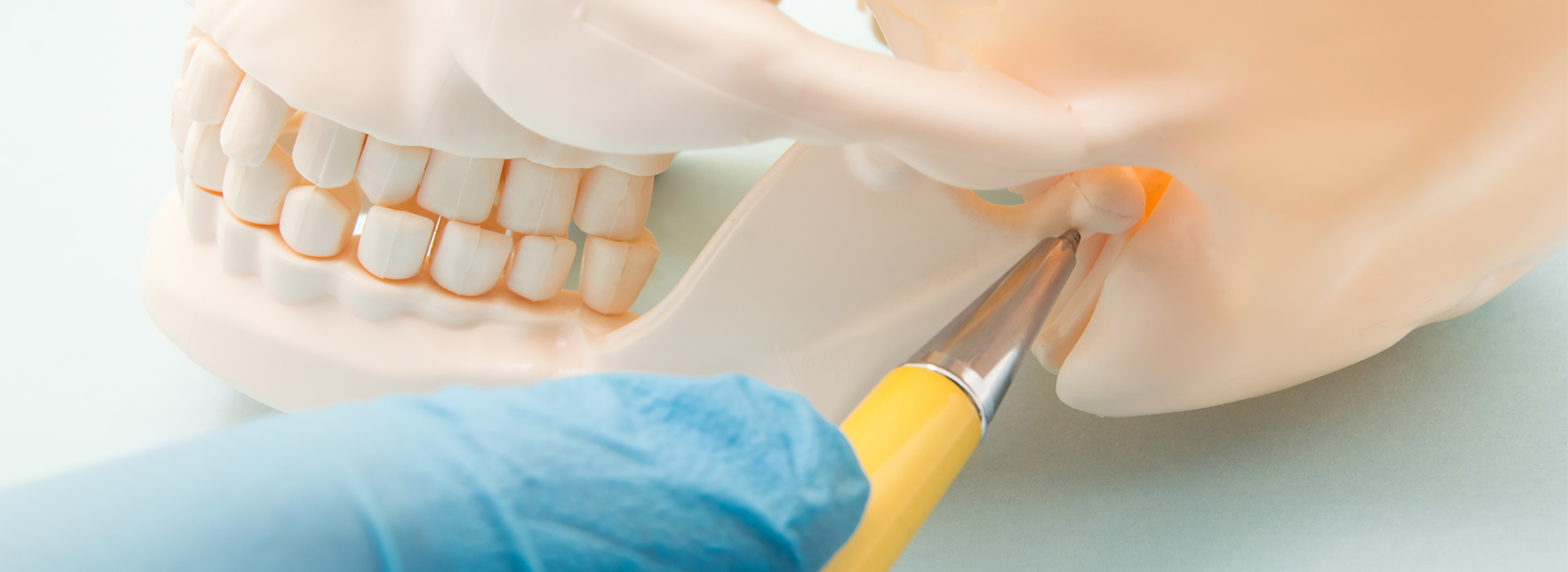
The temporomandibular joints (TMJs) are small but remarkably intricate connections that let your lower jaw move in multiple directions—up and down, forward and back, and side to side. Each joint couples a rounded condyle of the mandible with a socket in the temporal bone and contains a soft, fibrous disc that cushions movement. Because the joint works together with a network of muscles, ligaments and tendons, even small changes in one structure can affect the whole system.
That combination of hinge-like rotation and sliding translation is what makes the TMJ one of the most complicated joints in the body. Its complexity explains why jaw problems can present in so many different ways and why a careful, systematic approach is essential when symptoms appear. Rather than a single malfunction, TMJ disorders often reflect an imbalance among the joint surfaces, the supporting disc, and the surrounding musculature.
Although TMJ disorders are common, they don’t always follow a single pattern. For some people the issue is mainly muscular, for others it’s an internal joint problem, and in other cases degenerative changes are the driver. Recognizing which component is involved guides both diagnosis and treatment planning, which is why a targeted evaluation is so important.
TMJ problems can have many origins. Chronic teeth grinding or clenching (bruxism) places continual stress on the joint and surrounding muscles, which can lead to pain and wear over time. Trauma—such as a blow to the jaw or whiplash—can also disrupt the joint’s anatomy and lead to persistent dysfunction. In addition, systemic conditions like rheumatoid arthritis may produce inflammatory changes in the joint that contribute to pain and limited movement.
Behavioral and lifestyle factors also play a role. Excessive gum chewing, frequent wide yawning, or sustained poor posture can exacerbate symptoms by increasing strain on the muscles and ligaments that support the TMJ. Stress is another common contributor because it often leads to unconscious clenching or tightening of the jaw muscles, particularly during sleep.
Some people may be predisposed to TMJ problems because of their bite relationship or dental wear patterns. While malocclusion alone doesn’t guarantee a disorder, it can influence how forces are distributed across the joint and the teeth. Understanding each patient’s unique mix of risk factors helps shape practical, individualized care plans focused on relief and long-term stability.
TMJ disorders can produce a wide range of signs, and the same condition may affect different people in different ways. Common complaints include jaw pain or tenderness, aching around the ear, and difficulty chewing. You might also notice clicking, popping or a grating sensation when opening or closing the mouth, or episodes where the jaw locks in an open or closed position.
Because the muscles and joints around the jaw are connected to the head, neck and ears, TMJ problems often cause symptoms in nearby areas. Patients frequently report headaches, ear fullness or ringing (tinnitus), and neck or shoulder discomfort. These overlapping symptoms can make it challenging to identify the TMJ as the source without a focused examination.
If symptoms are interfering with daily activities—sleep, eating, speaking, or concentrating—it's time to seek evaluation. Early diagnosis can prevent escalation and often allows for more conservative treatment options to be effective. Even intermittent or mild symptoms deserve attention when they persist or worsen over time.
Diagnosis starts with a careful clinical assessment. A clinician will review your history, ask about symptom patterns and timing, and observe jaw motion and muscle function. Palpation of the joint and surrounding muscles helps identify areas of tenderness or abnormal movement. Simple functional tests—like measuring how wide you can open or noting deviations in jaw motion—provide additional clues.
Imaging and diagnostic tests are used selectively to clarify the problem. Panoramic X-rays, CBCT (cone beam computed tomography), and MRI can reveal different elements of joint structure and soft-tissue health. MRI is particularly useful when disc position or internal joint derangement is suspected because it visualizes soft tissues and disc-condyle relationships. These tools are used judiciously to confirm clinical impressions and to guide treatment decisions.
Because TMJ conditions often involve both muscular and joint components, a comprehensive evaluation may also include assessment of sleep habits, bruxism behaviors, and overall dental occlusion. Collaboration with or referral to specialists—such as oral surgeons, physical therapists, or pain management experts—may be appropriate when symptoms are complex or when advanced interventions are being considered.
Many patients experience meaningful improvement through conservative measures that reduce strain and promote muscle relaxation. Short-term strategies typically include eating a soft diet, avoiding wide or repetitive jaw movements, applying ice or moist heat as appropriate, and practicing stress-reduction techniques that reduce clenching. Gentle, guided stretching exercises can restore mobility when used under professional instruction.
Oral appliances are a cornerstone of noninvasive clinical care. Custom night guards or stabilization splints help redistribute forces, protect teeth from grinding, and reduce abnormal loading of the joint. These devices are tailored to the individual and adjusted as symptoms change. When inflammation is a significant factor, targeted medication prescribed by a clinician may provide short-term relief and improve comfort enough to allow rehabilitation exercises to be effective.
For cases that do not respond to conservative care, more advanced interventions may be considered. Procedures range from minimally invasive joint injections to arthrocentesis and, in rare and carefully selected situations, surgical correction. The choice of intervention depends on the underlying diagnosis, symptom severity, and the patient’s overall health and goals. Throughout, the emphasis is on meaningful symptom relief and restoring reliable function with the least invasive, most predictable approach possible.
At Ballston Dental Center, we approach TMJ disorders with a focus on careful assessment and individualized care. If jaw pain, clicking, or limited movement are affecting your daily life, our team can evaluate your situation and recommend a treatment plan tailored to your needs. Contact us to learn more or to schedule an evaluation—our goal is to help you regain comfort and normal jaw function.

The temporomandibular joints (TMJs) connect the lower jaw to the skull and permit complex movements such as opening, closing and side-to-side motion. Dysfunction of the joint, its cushioning disc or the surrounding muscles can cause pain, limited opening and noises like clicking or popping. When the joint and muscles are not working in balance, normal tasks such as chewing and speaking can become uncomfortable or difficult.
TMJ disorders often reflect a combination of muscular, joint and structural factors rather than a single isolated problem. Identifying which component is involved helps clinicians select treatments that address the root cause. A careful, systematic assessment increases the chance that conservative therapies will restore reliable function.
Common signs include jaw pain or tenderness, aching around the ear, difficulty chewing and audible clicking or popping during mouth movement. Patients may also experience episodes where the jaw partially locks or deviates when opening, and some notice increased tooth sensitivity or wear from altered bite patterns. Because the TMJ connects with muscles that extend into the head and neck, symptoms frequently overlap with headaches, neck pain and ear sensations.
Ear-related complaints can include fullness, pressure or ringing that mimic ear conditions but actually originate from the TMJ region. Symptoms that interfere with sleep, eating or daily function warrant prompt evaluation. Even intermittent discomfort should be assessed if it persists or progressively limits activity.
TMJ problems have multiple potential causes, including chronic teeth grinding or clenching (bruxism), direct trauma to the jaw, and inflammatory joint conditions such as rheumatoid arthritis. Behavioral and lifestyle contributors like excessive gum chewing, frequent wide yawning or sustained poor posture can increase strain on the joint and supporting muscles. Emotional stress is another common factor because it often leads to increased jaw muscle tension, especially during sleep.
Anatomical factors such as malocclusion or patterns of dental wear may predispose someone to abnormal force distribution across the joint, although bite relationships alone do not guarantee a disorder. Age-related degenerative changes can also play a role in some patients. Understanding a patient’s unique mix of mechanical, systemic and behavioral risk factors helps shape an individualized care plan.
Evaluation begins with a thorough history and focused clinical examination, including observation of jaw motion, palpation of the joint and muscles, and assessment of bite relationships. Clinicians will measure range of motion, note deviations or locking, and test for areas of tenderness to distinguish muscular from internal joint problems. A review of sleep habits and bruxism behaviors is often included to identify contributing factors.
Diagnostic imaging is used selectively to clarify findings and guide treatment: panoramic X-rays and CBCT reveal bony anatomy while MRI visualizes soft tissues and disc position when internal derangement is suspected. These tools complement the clinical exam rather than replace it and are chosen based on the suspected diagnosis. Collaboration with specialists such as oral surgeons, physical therapists or pain management clinicians may be recommended for complex presentations.
Most treatment approaches start with conservative measures aimed at reducing strain and promoting muscle relaxation, including a soft diet, avoiding wide or repetitive mouth opening, and using ice or moist heat as appropriate. Short-term behavioral adjustments such as reducing gum chewing, practicing jaw-resting postures and learning stress-reduction techniques can significantly lower muscle tension. Gentle, guided stretching and strengthening exercises taught by a clinician or therapist help restore mobility and function.
When inflammation contributes to symptoms, clinicians may recommend short courses of targeted medications to improve comfort and permit rehabilitation exercises to be effective. Education about sleep habits and nighttime clenching is also important, since reducing bruxism behavior can prevent ongoing joint overload. The goal of conservative care is meaningful symptom relief while minimizing invasive interventions.
Custom-made oral appliances, such as stabilization splints or night guards, are commonly used to redistribute forces, protect teeth from grinding and reduce abnormal loading of the TMJ. These devices are fabricated to fit the individual patient and are adjusted as symptoms change, allowing clinicians to modify the bite relationship and muscle activity safely. By reducing parafunctional forces, appliances often decrease muscle pain and protect joint structures while other therapies take effect.
Oral appliances are most effective when combined with behavioral strategies and therapeutic exercises, and they are not a universal solution for every TMJ diagnosis. Regular follow-up is necessary to monitor appliance fit, symptom response and any changes in dental or joint status. If an appliance is ineffective after a reasonable trial, clinicians will reassess the diagnosis and consider alternative or adjunctive treatments.
Minimally invasive interventions such as corticosteroid or hyaluronic acid injections and arthrocentesis can be useful when joint inflammation or internal derangement fails to respond to conservative care. These procedures are intended to reduce inflammation, improve joint lubrication and relieve pain, often enabling patients to participate more effectively in rehabilitation. They are typically performed only after a careful diagnostic workup confirms the specific joint pathology that injections can address.
Surgical options, including arthroscopy or open joint surgery, are reserved for a small subset of patients with persistent structural problems that do not respond to less invasive therapies. The decision to pursue surgery is made collaboratively and considers symptom severity, imaging findings and the patient’s overall health and treatment goals. When surgery is indicated, the emphasis remains on predictable restoration of function with the least invasive, most appropriate technique.
Yes; the muscles and nerves that serve the jaw are closely connected to the head, ears and neck, so TMJ dysfunction commonly produces referred pain in these areas. Patients often report tension-type headaches, a sense of ear fullness or ringing, and stiffness or soreness in the neck and shoulders in association with jaw symptoms. These overlapping manifestations can make diagnosis challenging without a focused, region-specific evaluation.
Recognizing the pattern of referred pain is an important part of assessment because treating only the apparent symptom, such as a headache, may not resolve the underlying TMJ problem. A comprehensive evaluation that includes jaw function, muscle palpation and appropriate imaging helps determine whether the TMJ is the source. Addressing the primary jaw disorder frequently reduces the secondary head, ear and neck complaints.
Your initial visit will include a detailed history and a focused clinical exam to assess jaw movement, muscle tenderness and bite relationships, along with questions about sleep habits and any history of trauma. The clinician may perform functional tests such as measuring maximum opening and observing deviations, and will palpate the muscles and joints to localize pain. If indicated, imaging such as panoramic X-rays, CBCT or MRI will be recommended to clarify structural or soft-tissue findings.
Based on the findings, the team will discuss a tailored plan that prioritizes conservative measures and outlines potential next steps if additional interventions become necessary. The process emphasizes clear explanation of the suspected cause, expected outcomes of recommended therapies and a follow-up schedule to monitor progress. This systematic approach helps ensure care is targeted and evidence based.
Long-term management focuses on reducing repetitive strain, improving posture, and addressing parafunctional habits such as teeth grinding and clenching. Practical strategies include maintaining a soft diet during flare-ups, avoiding extreme mouth opening, practicing jaw relaxation techniques and following a clinician-recommended exercise program to maintain mobility and muscular balance. Consistent attention to sleep hygiene and stress management also helps minimize episodes of increased muscle tension.
Regular dental checkups enable monitoring of occlusion and dental wear patterns that can influence joint loading, and timely intervention for bruxism or bite changes can reduce future risk. If ongoing or recurrent symptoms persist despite self-care, consult the practice in Arlington, Virginia so clinicians can reassess the condition and adjust the treatment plan. Early, targeted care improves the likelihood of sustained symptom control and functional stability.
We are here to help you take the next step toward a healthier smile.
Whether you have questions about our services, insurance, or scheduling your first visit, our team is ready to assist you.
We welcome new and returning patients and are happy to help you find a time that fits your schedule. Reach out to our office today to schedule an appointment or learn more about how we can support your oral health. We look forward to welcoming you to our practice.