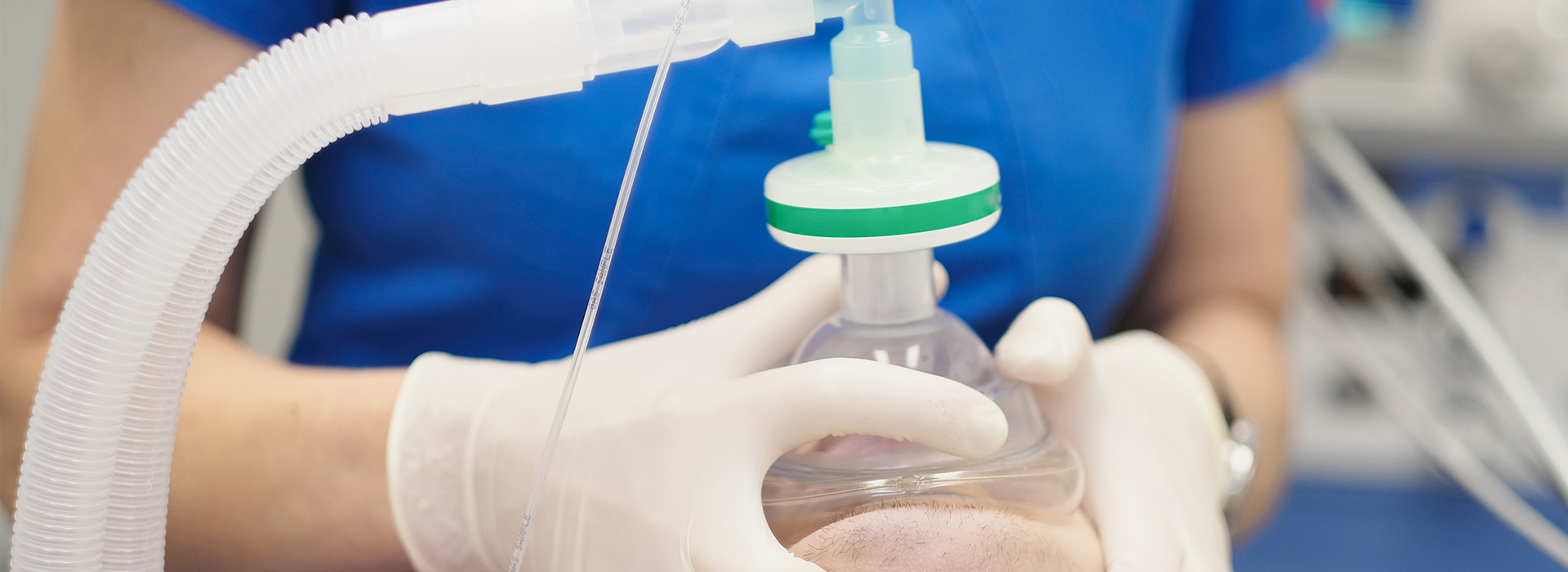
Anxiety about dental visits is common — many adults and children feel nervous before a checkup or a procedure. If fear or worry keeps you from getting the care you need, the team at Ballston Dental Center can help you find a more comfortable path to better oral health. We offer a range of sedation options delivered with careful monitoring and professional oversight so patients can get necessary treatment without excessive stress.
Avoiding the dentist because of fear can lead to worsening problems that require more invasive care later on. Sedation dentistry is not about escaping treatment; it’s about making treatment manageable. By reducing the physical and emotional barriers to care, sedation helps patients stay on track with preventive visits and complete required procedures with less trauma.
Our approach focuses on safety, clear communication, and individualized planning. Before recommending any sedation method, we review medical history, discuss goals and concerns, and explain what to expect — so you can make an informed decision and feel confident about your visit.
Sedation dentistry works by lowering anxiety and promoting relaxation so that a dental visit feels less stressful. Depending on the method, sedation can ease nervousness, blunt the memory of the procedure, and allow patients to remain calm and cooperative while care proceeds. For many people, that difference is what makes routine maintenance and essential treatment possible.
Even when sedation is used, local anesthesia is typically applied to numb the treatment area and prevent pain. Sedation addresses the emotional side of care — fear and tension — while local anesthetic handles sensation. That combination lets clinicians work more efficiently and patients experience less discomfort during and after treatment.
Importantly, sedation is adjusted to the needs of each person. Our dental team tailors the level and type of sedation to the nature of the procedure, the patient’s medical background, and their comfort goals. The result is a more controlled, predictable experience for both patient and provider.
People seek sedation for many reasons beyond generalized nervousness. Some patients have strong, long-standing dental phobias that interfere with routine care. Others find specific procedures — extractions, root canals, or lengthy restorations — especially difficult to tolerate. Sedation can make these visits feasible without unnecessary distress.
Sedation is also helpful for patients who struggle with a sensitive gag reflex, hypersensitive teeth and gums, or dental conditions that make it hard to stay comfortably in the chair. By reducing reflexive responses and sensory overload, sedation allows clinicians to work safely and accurately.
For children, individuals with special needs, or patients who have difficulty remaining still due to medical or cognitive conditions, appropriate sedation enables completion of necessary treatment in fewer visits. That can reduce overall disruption and improve long-term oral health outcomes.
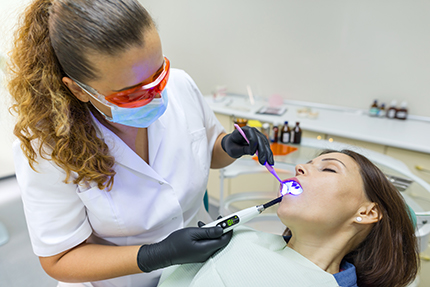
There is no single “right” way to sedate a patient; instead, a spectrum of options exists to match the level of anxiety and complexity of the procedure. At Ballston Dental Center, our goal is to recommend the least invasive method that still achieves a calm, safe visit. We’ll explain each option so you can weigh the benefits and practical considerations.
Sedation can be broadly divided into conscious approaches — where patients remain responsive to voice and touch — and deeper methods that require more intensive monitoring. For routine dental work, conscious sedation is usually sufficient and offers a favorable safety profile when administered by trained professionals.
Choosing among options depends on medical history, medications, the expected length of the procedure, and patient preference. Our team discusses these factors openly and outlines any preparatory steps required for a smooth, well-supervised visit.
Conscious sedation produces relaxation without eliminating the ability to follow simple instructions. Patients may feel drowsy, calm, or even drift in and out of awareness, yet they can usually respond when spoken to. Because breathing and basic reflexes are preserved, this level of sedation can be delivered safely in the dental office for many procedures.
Deeper anesthesia — often provided in a hospital setting by an anesthesiologist — places patients in a medically induced sleep and is reserved for cases where other methods are insufficient. Such care is appropriate for highly complex surgeries or when a patient's health or behavioral needs require a controlled operating-room environment.
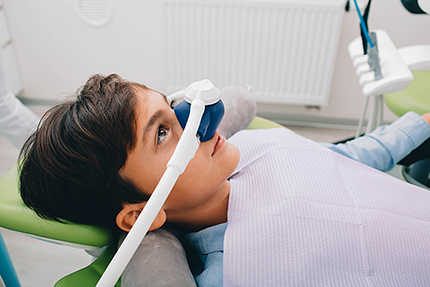
Nitrous oxide, commonly called “laughing gas,” is a mild, fast-acting gas delivered through a small nasal mask. It reduces anxiety and helps patients relax while maintaining responsiveness. Effects dissipate quickly after the gas is stopped, allowing a rapid return to normal awareness. Nitrous oxide can be an excellent option for patients with mild to moderate anxiety and those who need help reducing gag reflexes.
Oral sedatives are taken before the appointment and produce a deeper sense of calm. These medicines can make patients very drowsy and less aware of the procedure, though most remain able to respond to verbal cues. Because oral medications can linger in the system, patients receiving this type of sedation should arrange for a responsible adult to accompany them to and from the visit.
IV sedation allows precise control over sedation depth and acts quickly. It is used when more significant relaxation is needed for longer or more involved procedures. Because IV sedation affects alertness and may require fasting beforehand, careful pre-visit instructions and a companion to drive home afterward are standard precautions for safety and comfort.
Safety is the foundation of any sedation plan. Before recommending sedation, our clinicians take a thorough medical history, review current medications and allergies, and assess any conditions that could affect sedation choices. Clear communication about your health helps us select the safest approach.
We will provide specific pre-procedure instructions when sedation is part of your plan. These may include guidance about eating and drinking before the appointment, medication adjustments, and arranging transportation. Following these guidelines reduces risks and supports a smoother recovery.
During treatment, patients are monitored for breathing, heart rate, and blood oxygen levels, and trained staff remain vigilant throughout the visit. Aftercare instructions cover rest and activity restrictions until full awareness returns, and we explain signs that would warrant a prompt follow-up appointment or call.
On the day of treatment, we take time to answer questions and review consent and safety steps. Monitoring equipment is applied, and your comfort is checked continually. For conscious sedation methods, you will typically be able to follow simple instructions while feeling calm and relaxed.
After the procedure, recovery time varies depending on the sedation used. With nitrous oxide, recovery is rapid and most patients feel able to resume normal activities soon after. Oral and IV sedatives can require a longer period of observation and rest. In all cases, planning for a responsible escort home when required is part of our standard protocol.
We also schedule follow-up communication or visits as needed to confirm healing and address any questions. If anything about your recovery feels unusual, our team encourages you to reach out so we can provide guidance or arrange an extra check-in.
In summary, sedation dentistry is a practical, well-regulated way to reduce fear and enable necessary dental care with greater comfort and control. If dental anxiety or other factors make treatment difficult, our experienced team can explain your options and recommend a plan tailored to your needs. Contact us to learn more about sedation choices and how we can help you get the dental care you deserve.

Sedation dentistry offers patients with general anxiety or fears about a dental procedure the opportunity to have a more comfortable and stress-free experience. By utilizing safe and controlled sedation techniques, the patient is eased into a state of complete relaxation before the procedure. This approach eliminates discomfort, pain, and preoperative anxiety, and typically makes patients feel more at ease post-operatively, as they have little or no memory of the actual moment-to-moment procedure.
Local anesthesia involves an injection directly into or close to the area where a procedure is being performed. While it eliminates any sensation of pain in the targeted area, it does not affect your state of mind or level of anxiety. When a patient receives sedation, additional medications to ease anxiety and promote relaxation are employed in advance of local anesthesia. In this way, both the stress and discomfort associated with a procedure are eliminated. Sedation can be administered in a variety of forms based upon patient needs and the recommendations of the dentist or dental anesthesiologist.
Choosing the most appropriate method of sedation for a procedure depends on a variety of factors such as a patient's medical history and their level of anxiety. Dental sedation can come in the form of nitrous oxide sedation, oral conscious sedation, and IV sedation. Certain patients receiving comprehensive treatment or undergoing a complex surgical procedure may require general anesthesia in a hospital setting.
Nitrous oxide, or "laughing gas," is a mild sedative, which is inhaled through a small mask over the nose. A standard in dental sedation for decades, the effects of nitrous oxide are almost immediate and wear off quickly once your procedure is completed.
Oral sedation involves the prescription of an oral medication prior to your appointment. Taken at the recommended time before your visit, oral sedation allows you to feel fully relaxed by the time you're ready for your procedure. With oral sedation, it's necessary to plan on having an escort to and from your dentist's office.
IV Sedation is administered intravenously, or directly into a vein. It is typically indicated when a deeper state of sedation is required. Your dentist will provide you with specific instructions before your visit, and require that you have an escort for the trip home from your appointment.
Sedation dentistry uses medications to help patients relax during dental procedures, reducing anxiety and making treatment more comfortable. It ranges from mild calming agents, such as nitrous oxide, to deeper levels like oral or intravenous sedation that produce greater drowsiness. Sedation does not replace local anesthesia; clinicians still use numbing agents to prevent pain at the treatment site. The primary goal is to allow patients to receive necessary care with less stress and improved cooperation.
Sedation is individualized and selected based on the patient’s health, the procedure’s complexity, and personal comfort goals. Before any sedation is recommended, the dental team reviews medical history, current medications, and allergies to minimize risk. Patients are informed about what to expect and provide consent as part of the planning process. Safe monitoring and clear communication are central to a sedation visit.
Candidates often include people with dental anxiety or phobia, those who have avoided care for years, and patients who need lengthy or complex procedures. Sedation may also help individuals with a sensitive gag reflex, extreme dental sensitivity, or difficulty staying still because of medical or cognitive conditions. The dental team evaluates overall health, medications, and past reactions to sedation to determine suitability. Children and adults with special needs may be considered when sedation will enable safe, efficient care.
Not everyone requires the same level of sedation, and candidacy is determined case by case to prioritize safety. Patients who are pregnant, have certain cardiovascular or respiratory conditions, or take medications that interact with sedatives require special assessment. A thorough pre-visit review allows clinicians to recommend the least invasive option that will achieve the desired outcome. When questions or concerns exist, collaboration with a physician or anesthesiologist can be arranged.
Common in-office sedation options include inhalation sedation with nitrous oxide, oral sedation using prescribed medications, and intravenous (IV) sedation for greater control and rapid onset. Nitrous oxide is mild and short-acting, oral sedatives produce deeper relaxation, and IV sedation allows clinicians to adjust the level of sedation during longer or more involved procedures. Each method has distinctive benefits and monitoring requirements suited to different patient needs and treatment lengths.
The practice typically recommends the least intensive method that will meet the patient’s comfort and safety needs. Staff trained in sedation monitor vital signs such as heart rate and oxygen levels throughout the visit. Specific pre-appointment instructions, such as fasting requirements for deeper sedation, are provided based on the chosen approach. Proper preparation and supervision help ensure predictable, well-managed care.
Nitrous oxide is an inhaled sedative delivered through a small nasal mask that produces a calming effect without rendering patients unconscious. It works quickly to reduce anxiety and often helps decrease a sensitive gag reflex, making routine procedures easier to tolerate. The dental team adjusts the concentration to reach the desired level of relaxation while patients remain responsive to verbal cues. Once the gas is stopped, effects wear off rapidly and most patients regain normal awareness within minutes.
Because nitrous oxide wears off quickly, it is a convenient option for many procedures and requires minimal recovery time. Patients can typically resume normal activities without a companion after a short monitoring period, though individual responses vary. The dental team explains the process and monitors comfort and vital signs throughout the appointment. If nitrous alone is insufficient, clinicians may combine it with other conscious sedation methods when appropriate.
Preparation instructions vary with the type and depth of sedation but commonly include fasting for a specified period before IV or deeper oral sedation and arranging for a responsible adult to drive you home. Patients should provide a complete list of current medications, supplements, and medical conditions during the pre-visit review so the team can identify potential interactions or necessary medication adjustments. Avoiding alcohol and certain recreational substances for a recommended period before the appointment is important for safety. Clear directions from the office support a smooth, low-risk sedation experience.
Follow any specific instructions provided by the clinician, such as which medications to take or skip on the day of the procedure. Wear comfortable clothing and bring any required paperwork or identification. Plan for rest at home after deeper sedation, as alertness and coordination can remain impaired for several hours. If you have questions about preparation, call the office ahead of time to clarify guidance and ensure you are ready for your visit.
Sedation dentistry is generally safe when administered by trained professionals who follow established protocols, perform thorough pre-procedure evaluations, and monitor patients throughout the appointment. Safety measures include reviewing medical history and medications, checking vital signs such as heart rate and oxygen saturation, and having emergency equipment and trained staff available. The team chooses the lowest effective level of sedation for the procedure to minimize risk while maintaining comfort. In cases requiring deeper anesthesia, referral to a hospital setting or an anesthesiologist may be recommended.
Informed consent and clear communication are important components of safety, ensuring patients understand potential risks and aftercare expectations. Ongoing training and adherence to regulatory standards help keep sedation practices current and reliable. If any health changes occur between scheduling and the appointment, patients should notify the office so the sedation plan can be reassessed. Prompt follow-up is available if unexpected symptoms arise after a sedated visit.
Recovery varies by sedation type: nitrous oxide allows rapid recovery and most patients resume normal activities quickly, while oral and IV sedatives can produce longer-lasting drowsiness and slowed reflexes. For deeper forms of sedation, patients are usually observed until basic alertness and vital signs are stable and are advised to rest for the remainder of the day. A responsible adult should accompany anyone who receives oral or IV sedation to ensure safe transportation and initial post-procedure support at home.
The dental team provides specific aftercare instructions that cover activity restrictions, medication guidance, and warning signs that warrant a prompt follow-up. Avoid driving, operating heavy machinery, or making important decisions for the remainder of the day if you received moderate to deep sedation. Hydration, light meals once alert, and following prescribed pain-control measures help support a smooth recovery. If symptoms such as prolonged dizziness, difficulty breathing, or unusual bleeding occur, contact the office immediately for advice.
Sedation can be a valuable tool for children and patients with special needs when it enables necessary dental care to be completed safely and with minimal distress. The choice of sedation is guided by the patient’s age, medical history, level of cooperation, and the complexity of the procedure. For some pediatric patients, nitrous oxide or light oral sedation is sufficient, while others may require deeper sedation under stricter monitoring or in a facility equipped for advanced anesthesia.
The dental team tailors the approach to each patient, coordinating with parents, caregivers, and other healthcare providers as needed. Pre-visit planning addresses behavioral strategies, medication considerations, and post-procedure care to reduce complications and improve outcomes. Prior experience, underlying medical conditions, and communication needs are all considered when developing a safe, effective plan for vulnerable populations.
Determining the right sedation level involves evaluating the patient’s medical history, anxiety level, current medications, the expected duration and invasiveness of the procedure, and the patient’s personal preferences. The clinician aims for the least invasive method that will provide adequate relaxation and cooperation while maintaining safety. Pre-procedure screening and discussion allow the team to balance clinical needs with patient comfort and select an option such as nitrous oxide, oral medication, or IV sedation accordingly.
When higher-risk factors or more complex surgeries are present, the team may recommend deeper anesthesia administered in a controlled surgical setting or in partnership with an anesthesiologist. Clear explanations about risks, benefits, and required preparation help patients make informed choices. Ongoing monitoring allows clinicians to adjust sedation levels during the procedure as needed to maintain safety and comfort.
Begin by describing your fears, previous experiences with dental care or sedation, current medications, and any health conditions that might affect the choice of sedative. Ask about the specific methods available, what to expect before, during, and after sedation, and what monitoring and safety measures the office uses. Clear questions about fasting, transportation, and activity restrictions will help you plan the appointment and recovery. The dental team should explain alternatives and recommend the least invasive option that meets your needs.
If you prefer, request that the team outline step-by-step what will happen during the visit so you know when and how sedation will be administered and monitored. For more complex health situations, the office can coordinate with your primary care physician or an anesthesiologist to optimize safety. At Ballston Dental Center, our clinicians prioritize informed consent and open communication so patients can make confident decisions about sedation care.
We are here to help you take the next step toward a healthier smile.
Whether you have questions about our services, insurance, or scheduling your first visit, our team is ready to assist you.
We welcome new and returning patients and are happy to help you find a time that fits your schedule. Reach out to our office today to schedule an appointment or learn more about how we can support your oral health. We look forward to welcoming you to our practice.