If a dentist has recommended a root canal for one of your teeth, there’s no need for alarm. Modern root canal therapy is a well-established, predictable treatment designed to relieve pain, remove infection, and preserve the natural tooth whenever possible. Many patients are surprised to learn that the procedure is typically no more uncomfortable than having a routine dental filling.
At Ballston Dental Center, our focus is on clear explanations, gentle care, and using current technology to make treatment as efficient and comfortable as possible. We aim to help you keep your natural smile while protecting your long-term oral health.
Keeping a functional, natural tooth is often a better option than extraction when the tooth’s supporting structures are otherwise healthy. Root canal treatment removes damaged or infected tissue from inside the tooth, then seals the space so chewing function and appearance can be restored with a crown or other restoration. Preserving your tooth helps maintain proper chewing mechanics and prevents neighboring teeth from shifting.
Today’s techniques and materials make success rates for root canal therapy very high. When the tooth is properly diagnosed, treated, and restored afterward, it can remain comfortable and functional for many years — often for a lifetime. The goal is to treat the source of infection while minimizing disruption to the surrounding tissues.
Choosing root canal therapy also reduces the need for more invasive procedures later on. By intervening early, your dentist can often avoid extraction, bone loss, and the more complex restorative work that can follow a missing tooth.

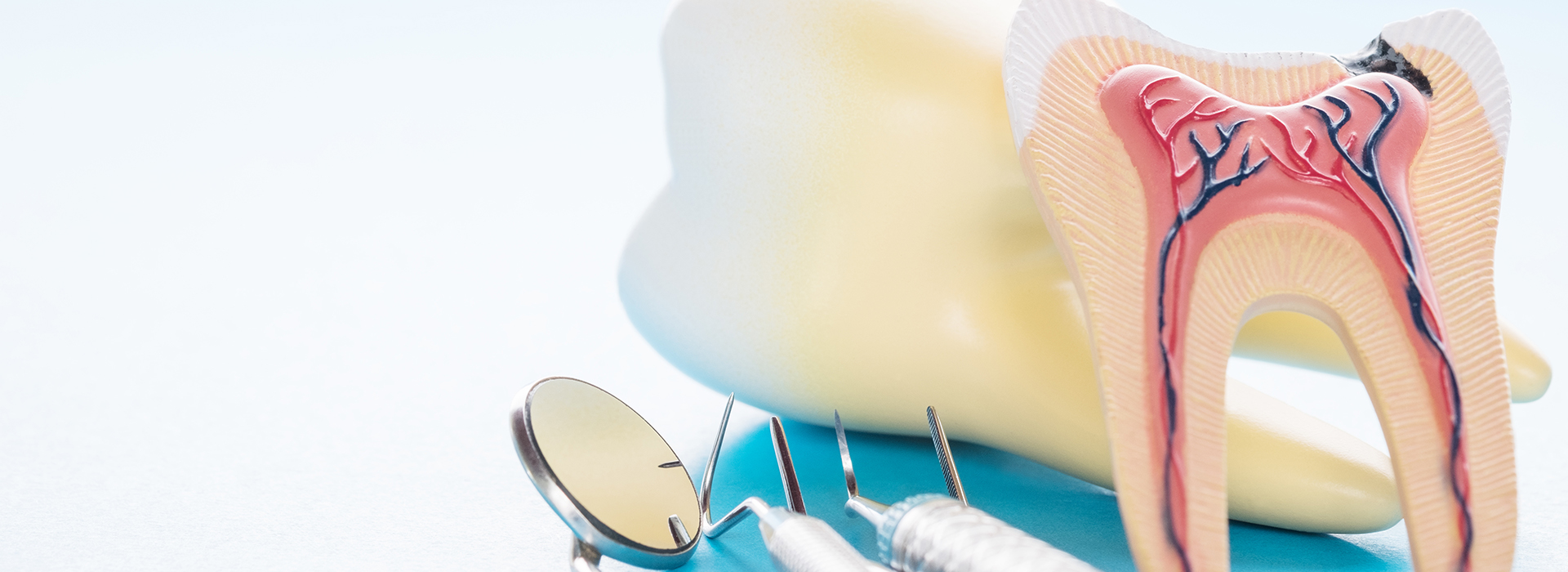
Inside each tooth lies the dental pulp — a small bundle of nerves and blood vessels that keeps the tooth alive during development. When decay, trauma, or repeated dental work breaches the outer layers of the tooth, bacteria can reach the pulp and trigger inflammation or infection. That process is what typically leads a clinician to recommend root canal therapy.
Symptoms can vary widely. Some patients experience sudden, intense toothache, while others notice only sensitivity to temperature or a gradual darkening of the tooth. In some cases there may be swelling, a small bump on the gum near the tooth, or no symptoms at all — with the problem discovered on a routine radiograph.
Because the signs can be subtle or mimic other dental conditions, prompt evaluation is important. Early assessment lets your dentist determine whether root canal therapy is the most appropriate option or if another treatment would better address the issue.
Although not every twinge or sensitivity means a root canal is required, the following are common indicators that the inner tissues of a tooth may be compromised:
Ongoing tooth pain that interferes with sleep or daily activities often signals deep decay or infection. Pain that intensifies when lying down or keeps you awake at night should be evaluated promptly.
Long-lasting or severe sensitivity to hot or cold that doesn’t resolve after the stimulus is removed can indicate inflamed or dying pulp tissue.
Discomfort on chewing, or pain when a tooth is lightly tapped, may point to nerve irritation or an underlying infection that requires treatment.
A tooth that becomes darker than the surrounding teeth after trauma or decay may have compromised internal tissues and merit evaluation.
A fractured tooth can expose the pulp to bacteria and lead to inflammation or infection; treating the interior of the tooth offers a way to retain it.
Localized swelling, sensitivity of the surrounding gum, or a persistent sore spot may indicate a spreading infection that should be addressed quickly.
If an infection has affected the supporting bone, the tooth can become slightly mobile. Root canal therapy combined with appropriate restoration and follow-up care can often arrest the process and promote healing.
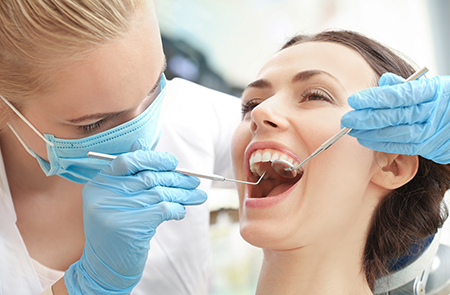
Delaying evaluation or treatment after you notice symptoms can allow infection to progress and potentially involve more of the surrounding bone and soft tissues. Early treatment tends to be less complex and more predictable. In many cases, intervening before the infection advances saves more of the natural tooth and reduces the need for additional procedures.
Root canal therapy also reduces the chance that an infection will spread to adjacent teeth or soft tissues. While the body mounts defenses against oral infections, uncontrolled spread can lead to more significant complications that require urgent care.
Regular dental examinations and timely radiographs are useful for identifying teeth that are at risk but not yet painful. These preventive evaluations let your dental team recommend the most appropriate treatment before symptoms escalate.
A contemporary root canal procedure follows a methodical sequence designed to clear infection and protect the tooth. Your dentist will begin with a thorough exam, appropriate imaging, and a discussion of the findings and treatment plan. Local anesthesia is used to ensure comfort, and sedation options are available if needed to help patients relax.
Once numb, the doctor creates a small opening in the crown of the tooth to access the infected pulp chamber and canal system. Specialized files and irrigation solutions are used to remove diseased tissue and disinfect the canals. The cleaned canals are then shaped and filled with a biocompatible material to seal the internal space.
Some teeth can be completed in a single visit; others require multiple appointments depending on complexity, the presence of infection, or anatomical considerations. After the root canal phase is finished, the tooth typically needs a permanent restoration — often a crown — to restore strength and function.
Recovery from a root canal is usually straightforward. It’s common to experience some soreness or tenderness for a few days as surrounding tissues settle and heal. Over-the-counter pain relievers are effective for most patients, and your dentist will advise on appropriate options and any prescription needs.
After treatment, protecting the tooth with a timely permanent restoration is important. A crown or similar restoration restores chewing function and guards against fracture — a restored tooth is much more resilient and predictable long term. Until that restoration is in place, take care to avoid heavy chewing on the treated side.
Maintaining excellent oral hygiene and keeping routine dental visits helps ensure that the treated tooth remains healthy. On occasion, a root canal-treated tooth can need retreatment if new issues arise; prompt attention to any recurring symptoms helps your dental team identify concerns early.
Aftercare tips to support healing and long-term success:
After anesthesia, avoid chewing or touching the treated side until normal sensation returns to prevent accidental injury to soft tissues.
Mild to moderate soreness is normal for a few days; it should diminish steadily. Use recommended pain relief and reach out if discomfort worsens or persists.
If antibiotics are prescribed to address infection, take the full course exactly as directed to support complete healing.
Temporary fillings can be vulnerable to fracture. Avoid hard, sticky foods and try to chew on the opposite side until your permanent restoration is placed.
Continue brushing and flossing gently but thoroughly around the treated tooth to keep surrounding tissues healthy and to prevent new problems.
Plan to restore the tooth with a crown or appropriate permanent restoration as recommended so you can regain full function and long-term protection.
Root canal therapy is a conservative, effective way to relieve pain and retain a tooth that would otherwise need removal. If you’re experiencing symptoms or if your dentist has advised treatment, timely care improves the chances of a comfortable outcome and long-lasting results. Contact our office to learn more or to arrange an evaluation — we’re happy to answer your questions and help you take the next step toward a healthy smile.

A root canal procedure is the best way to save a tooth that has been damaged by decay or injury and preserve your natural smile. The alternative is an extraction and treatment to replace the tooth. While at times a tooth is non-restorable and an extraction is the only option, when possible, it’s best to try and save your natural tooth. With proper care, a tooth with root canal therapy can serve your smile well for many years to come.
Despite lingering myths from before the age of modern dental anesthesia and technology, having a root canal procedure today is as routine and comfortable as visiting the dentist for a filling. While the procedure is performed under local anesthesia with your tooth completely numbed, we can also discuss options in dental sedation.
Whether the symptoms of a dental infection subside after a course of antibiotics, a draining abscess provides you with some temporary pain relief, or a tooth with radiographic evidence of pathology has not yet developed symptoms, it’s essential, before an infection worsens or occurs, to have a root canal procedure performed. In this way, the tooth can be disinfected, filled, and sealed to protect your health and avoid further problems.
If you have sustained a dental injury, have a toothache, jaw pain, swelling, or are experiencing any other unusual and uncomfortable oral symptoms, contact our office immediately for care. Dental problems that have not been evaluated and treated can significantly worsen, producing more severe damage and consequences for the involved teeth, your oral health, and even your overall wellbeing. Once you get in touch with our office, our friendly and compassionate office team will get you in for care at your earliest convenience.
While some root canal procedures can be completed in one visit, others may involve 2 or 3 appointments. How long it takes depends on various factors, including active infection, the number of canals in the tooth, and the tooth’s location or anatomy.
With a success rate that exceeds 95%, root canal therapy remains the most effective procedure to save a tooth in which the inner vital tissues have been damaged. However, as with all healthcare procedures, there are a small percentage of cases where the teeth become symptomatic a second time. The good news is that many of these teeth can still be saved with root canal retreatment or a minor surgical procedure known as an apicoectomy.
The best ways to maintain a tooth with root canal therapy are to get the proper restoration required to rebuild and protect the tooth, maintain proper oral hygiene, and schedule appointments for routine dental checkups and care.
Saving a tooth with root canal therapy is a wise investment that, in the long run, is typically less costly and invasive than having the tooth extracted and replaced with a fixed bridge or implant. As far as the exact cost of care, it can vary depending on which tooth is being treated. Many dental insurance plans provide coverage for root canal therapy. At the office of Ballston Dental Center, we do our best to optimize your dental benefits and minimize your out-of-pocket expenses. Our staff will answer all your questions about the cost of care and discuss all your payment options.
At the office of Ballston Dental Center, we use the latest technology and most effective methods of care to provide precise and gentle care. Our reputation for excellence is based upon a consistent record of achieving successful treatment outcomes while providing prompt, stress-free, and convenient treatment for every type of dental need.
Root canal therapy is a dental procedure that removes infected or inflamed pulp from inside a tooth, cleans and disinfects the canal system, and seals it to prevent reinfection. The treatment is designed to eliminate pain and stop the spread of infection while preserving the natural tooth whenever possible. Dentists recommend this therapy when decay, trauma, or repeated dental work has compromised the inner tissues and left the tooth at risk of abscess or progressive damage.
The primary goals are pain relief, infection control, and restoration of function. Preserving the natural tooth helps maintain chewing mechanics and prevents adjacent teeth from shifting, which supports long-term oral health. When properly diagnosed and restored, a treated tooth can remain functional for many years.
Pulp damage most often results from deep decay, a fracture or crack that exposes the inner tissue, or a forceful impact to the tooth. Bacteria penetrating those pathways can inflame or infect the pulp, producing a range of clinical presentations. Repeated dental procedures in the same area or untreated cavities also increase the risk of pulp compromise.
Symptoms can vary from sudden, severe toothache to lingering sensitivity to hot or cold, pain when biting, or a gradual darkening of the tooth. Some patients develop swelling or a small bump on the gum near the affected tooth, while others have no symptoms and the problem is discovered on a routine X-ray. Prompt evaluation is important because early detection often leads to simpler, more predictable treatment.
Determining the need for root canal therapy begins with a thorough clinical exam, a review of your symptoms and dental history, and diagnostic imaging such as periapical radiographs or CBCT when indicated. Dentists may perform tests to assess vitality, percussion sensitivity, and the pattern of pain to distinguish nerve-related issues from other causes. This diagnostic process helps ensure the correct tooth and problem are identified before treatment is recommended.
In some cases, additional consultation with an endodontist is advised for complex anatomy or unclear findings. Accurate diagnosis guides treatment planning and helps the dental team decide whether conservative care, direct restoration, monitoring, or root canal therapy is the most appropriate approach for your situation.
Your appointment will typically begin with a review of findings, local anesthesia to ensure comfort, and placement of a rubber dam to isolate the tooth and keep it dry. The dentist makes a small opening in the crown to access the pulp chamber, then uses specialized instruments and irrigants to remove infected tissue, disinfect the canals, and shape the space for a permanent seal. Many practices use digital imaging and magnification to improve precision and predictability.
Once the canals are cleaned and filled with a biocompatible material, the tooth may receive a temporary or permanent restoration depending on the case. Some teeth can be completed in a single visit while others require multiple appointments; ultimately a full coronal restoration, often a crown, is recommended to restore strength and protect the treated tooth from fracture.
Modern root canal procedures are performed under local anesthesia, and most patients report that the treatment feels similar to having a routine filling. Dentists take steps to keep you comfortable, including offering sedation options for those with significant anxiety. During the procedure you should not feel sharp pain, though you may sense pressure or movement.
After treatment it is common to experience mild to moderate soreness for a few days as surrounding tissues heal, and over-the-counter pain relievers are effective for most patients. If pain increases, swelling develops, or symptoms persist beyond the expected recovery period, contact the dental team promptly for evaluation and care.
The primary alternative to root canal therapy is extraction of the affected tooth followed by a restorative option such as a dental implant, fixed bridge, or removable prosthesis. Each replacement option has different clinical considerations related to adjacent teeth, bone preservation, and long-term function; your dentist can explain the pros and cons for your situation. In some cases, conservative measures such as pulp capping or monitoring may be possible for early or reversible pulp injuries.
When a tooth cannot be maintained with conventional treatment, surgical options such as an apicoectomy may be considered to address persistent infection at the root tip. Decisions about alternatives should be individualized based on the tooth’s condition, overall oral health, and the most predictable path to long-term stability.
Immediately after treatment avoid chewing on the treated side until the tooth is permanently restored, since temporary fillings can be vulnerable to fracture. Expect some tenderness and follow the dentist’s recommendations regarding pain management and any prescribed medications. Good oral hygiene is important to keep surrounding tissues healthy while healing progresses.
Recovery time varies but most patients feel substantially better within a few days and return to normal function as the discomfort subsides. It is important to schedule the recommended restorative follow-up, often a crown, to protect the tooth and restore full chewing strength. Regular dental visits and proper maintenance help ensure long-term success.
Root canal treatment has a high success rate when the tooth is properly diagnosed, treated thoroughly, and restored with an appropriate permanent restoration. Many treated teeth remain comfortable and functional for decades, and some last a lifetime with good care. Success depends on factors such as the extent of infection, tooth anatomy, the presence of cracks or fractures, and the quality of the final restoration.
Occasionally a treated tooth may require retreatment or surgical intervention if new problems arise or if the original treatment did not fully resolve the issue. Timely management of recurring symptoms and consistent follow-up care improve the chances of preserving the tooth long term.
You should seek prompt dental attention if you experience severe or worsening pain, persistent swelling of the face or jaw, difficulty breathing or swallowing, or fever in combination with dental symptoms. These signs can indicate a spreading infection that requires immediate evaluation. A sudden increase in pain after treatment or the development of a hard, painful swelling merits urgent review by your dental team.
If you notice unexpected drainage, a rapidly growing lump on the gum, or sudden loosening of the treated tooth, contact your dentist without delay. Early intervention often prevents complications and helps direct the most appropriate next steps for care.
Most root canals are completed with local anesthesia, which numbs the area and minimizes pain. For patients who experience anxiety or require additional relaxation, options commonly include nitrous oxide (laughing gas), oral conscious sedation, or intravenous sedation depending on medical history and case complexity. Your dentist will review available choices and recommend the safest, most suitable approach for comfort during treatment.
Discuss your anxiety level, past experiences with dental care, and any medical conditions or medications with the dental team so they can tailor a plan that prioritizes safety and comfort. If you prefer, the staff at Ballston Dental Center can explain sedation options and help coordinate care to make the appointment as relaxed as possible.
We are here to help you take the next step toward a healthier smile.
Whether you have questions about our services, insurance, or scheduling your first visit, our team is ready to assist you.
We welcome new and returning patients and are happy to help you find a time that fits your schedule. Reach out to our office today to schedule an appointment or learn more about how we can support your oral health. We look forward to welcoming you to our practice.