Oral surgery covers a broad spectrum of procedures designed to restore oral function, relieve pain, and prepare the mouth for long-term restorative work. Whether addressing a wisdom tooth that won't erupt properly, stabilizing the jaw after trauma, or creating the ideal foundation for dental implants, surgical care in the mouth requires careful planning, experienced hands, and an emphasis on comfort and healing. Our approach blends clinical precision with clear communication so patients understand why a procedure is recommended and what to expect during recovery.
Not every dental problem can be resolved with a filling or a routine extraction. Some conditions—such as severely impacted wisdom teeth, teeth fractured below the gumline, or infections that do not respond to conservative therapy—require surgical intervention. In these situations, oral surgery can remove the source of pain or infection and prevent more serious complications, such as damage to adjacent teeth or spread of infection into nearby tissues.
Emergency oral surgery is also a critical element of comprehensive care. Facial or dental trauma, uncontrolled bleeding after an extraction, and acute infections that threaten airway or systemic health demand prompt surgical assessment and treatment. Our team evaluates each emergency with an eye toward stabilizing the patient first, then addressing the underlying surgical needs efficiently and compassionately.
Surgical endodontic procedures—often performed when conventional root canal therapy is insufficient—allow targeted treatment of persistent infection at the tip of a tooth’s root. By combining careful diagnosis with microsurgical techniques, these procedures aim to resolve chronic issues while preserving natural dentition whenever feasible.
Successful restorative dentistry frequently relies on preparatory surgical procedures to create a predictable foundation. Sinus lifts and bone grafts are common examples when the upper jaw lacks adequate bone to support an implant. By augmenting bone and reshaping the jaw, surgeons can provide the support needed for implants, crowns, and fixed prostheses to function comfortably for years.
Tissue recontouring and pre-prosthetic surgery focus on the soft tissues and bony contours that affect the fit and appearance of dentures, bridges, and crowns. These procedures can reduce sore spots, improve stability for removable prosthetics, and create more natural transitions between prosthetic restorations and surrounding gums, enhancing both comfort and aesthetics.
When dental implants are part of the restorative plan, precise surgical placement is essential. A well-executed implant surgery takes into account bone quality, occlusion (bite), and long-term maintenance. Properly placed implants preserve bone, support surrounding teeth, and allow for restorative work that looks and functions like natural teeth.
Surgical correction of jaw deformities is sometimes necessary to restore balanced function and facial harmony. Conditions that affect bite alignment or lead to chronic discomfort can often be improved through orthognathic procedures that reposition the jaws and realign dental occlusion. These surgeries are coordinated with orthodontic care when appropriate and emphasize both functional correction and predictable recovery.
Treatment for obstructive sleep apnea may include oral appliances or, in select cases, surgical approaches that open the airway. When conservative therapies do not provide adequate relief, surgical evaluation identifies anatomical contributors to airway obstruction and develops a plan tailored to the patient’s needs, always prioritizing safety and long-term outcomes.
Temporomandibular joint (TMJ) disorders span a range of functional problems from muscle-related pain to structural joint issues. For select cases where conservative measures are insufficient, surgical options can address joint pathology directly and reduce sources of chronic pain or dysfunction. Each surgical recommendation follows thorough clinical and imaging assessment so patients understand their options and likely benefits.
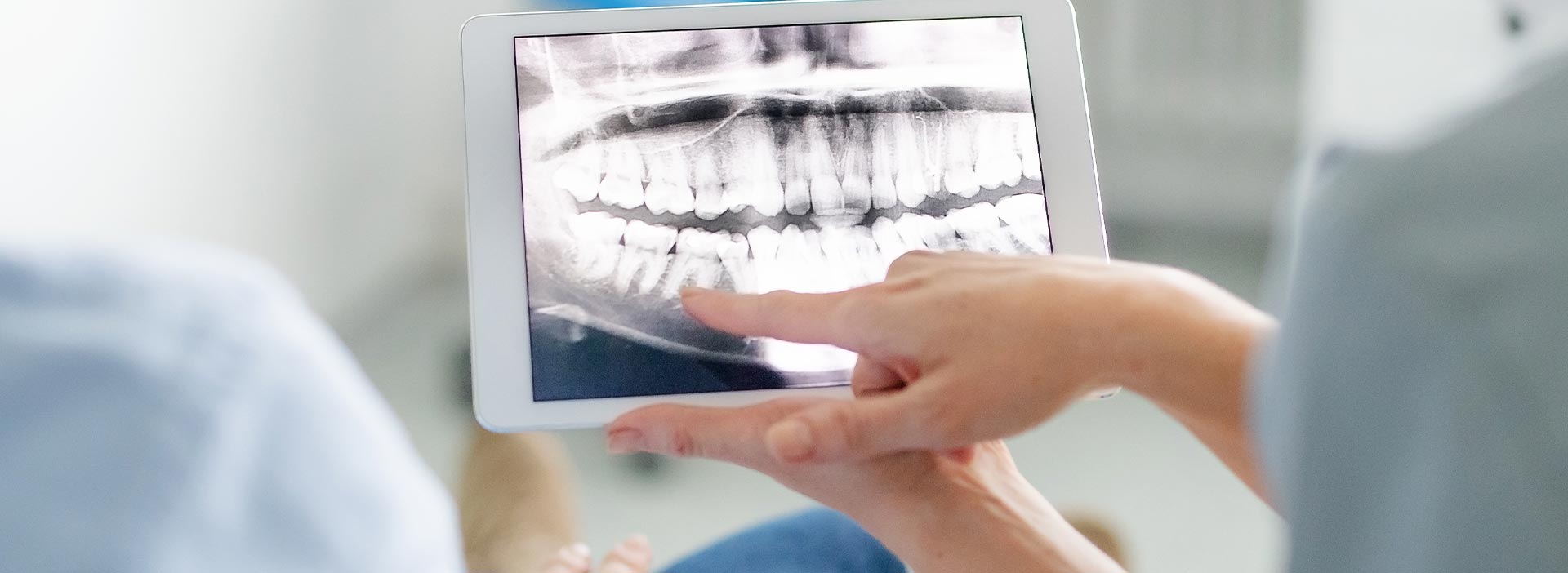
Advances in imaging and instrumentation have transformed how oral surgery is planned and performed. Three-dimensional imaging and cone-beam computed tomography (CBCT) allow clinicians to visualize bone, nerve pathways, and sinus anatomy in fine detail, reducing surprises during surgery and improving implant placement accuracy. These tools support predictable outcomes and safer treatment planning.
Minimally invasive surgical techniques—combined with magnification and microsurgical tools—reduce tissue trauma, minimize postoperative discomfort, and speed healing. When appropriate, sedation dentistry and carefully monitored anesthesia options help patients remain relaxed during procedures, and local anesthetic protocols keep pain under control during and after surgery.
Integrating digital planning with guided surgical templates can further enhance precision for implant placement and complex reconstructions. By mapping the ideal restorative position before incisions are made, the surgical team can execute treatment that aligns with the desired prosthetic result, optimizing both function and aesthetics.
Healing after oral surgery follows a predictable course, but individual experiences vary. In the immediate hours and days after a procedure, patients may notice swelling, mild discomfort, and changes in chewing or speech. Our team provides clear, personalized aftercare instructions—on wound care, diet, and activity level—to support smooth recovery and reduce the risk of complications.
Follow-up visits are an important part of the care plan. These appointments allow the clinician to monitor healing, remove sutures if necessary, and confirm that bone grafts or implants are integrating as expected. Timely follow-up also provides an opportunity to address questions and modify post-op care if healing deviates from the anticipated path.
Most patients resume normal activities within a few days to a couple of weeks depending on the complexity of the surgery. Pain management strategies emphasize safe, noninvasive measures and avoidance of anything that could interfere with clot formation or healing. Patients are advised on signs that warrant prompt attention—such as persistent bleeding, uncontrolled pain, or signs of infection—so issues can be handled quickly.
Throughout recovery, clear communication and accessible aftercare support help patients feel confident and informed. Our team collaborates with each patient to tailor postoperative instructions to their lifestyle and clinical needs, ensuring the best possible conditions for healing and long-term success.
At Ballston Dental Center, we approach oral surgery with a focus on thoughtful planning, gentle technique, and comprehensive aftercare so patients can return to comfortable, functional smiles. If you have questions about whether a surgical solution is the right fit for your dental needs, please contact us for more information and to discuss next steps.

Oral surgery encompasses a range of procedures performed to restore oral function, relieve pain, and prepare the mouth for restorative care. Common procedures include surgical tooth extractions, implant placement, bone grafting, and corrective jaw surgery. These treatments address problems that cannot be managed with routine dental care alone.
Surgical techniques vary from minimally invasive approaches to more complex reconstructive procedures, depending on the clinical needs. The goal is to preserve natural teeth when possible, alleviate infection or dysfunction, and create a stable foundation for long-term oral health. Decision-making is guided by clinical examination, imaging, and patient-centered planning.
Oral surgery is typically recommended when conservative treatments are unlikely to resolve the problem or when structural issues threaten adjacent tissues. Examples include severely impacted wisdom teeth, fractures extending below the gumline, persistent infections at the root tip, and anatomical deficiencies that prevent implant placement. Emergency scenarios such as facial trauma and uncontrolled post-extraction bleeding also require surgical assessment.
The surgical option aims to remove sources of pain or infection, stabilize the oral environment, and prevent further complications. Clinicians weigh risks and benefits and discuss alternatives like endodontic retreatment or prosthetic options when appropriate. Patient health status and goals factor into the final recommendation.
Bring a complete medical and dental history, a list of current medications, and any prior imaging or referral notes to the consultation. During the visit, the clinician will perform a focused exam, review imaging such as X-rays or CBCT scans, and discuss surgical indications and anticipated outcomes. You should also prepare questions about anesthesia, recovery, and how the procedure fits into your overall treatment plan.
At Ballston Dental Center in Arlington, clinicians strive to explain options clearly and create a coordinated plan with any needed specialists. The consultation may include a discussion of sedation choices and personalized preoperative instructions to ensure safety and optimal healing. Clear communication at this stage helps set realistic expectations and reduces anxiety.
Anesthesia choices range from local anesthesia to conscious sedation and, in select cases, general anesthesia, depending on the complexity of the procedure and patient needs. Local anesthesia numbs the surgical site, while nitrous oxide or oral sedatives can reduce anxiety and promote relaxation during office-based procedures. Intravenous sedation and general anesthesia may be recommended for longer, more invasive surgeries or for patients with special medical or psychological requirements.
The surgical team reviews your medical history and coordinates monitoring protocols to ensure safety throughout the procedure. Preoperative instructions will address fasting, medication adjustments, and transportation if sedatives are used. Postoperative pain control strategies are planned to minimize discomfort while protecting healing tissues.
Healing after oral surgery commonly involves swelling, mild to moderate discomfort, and changes in chewing or speech that resolve over time. Following postoperative instructions on wound care, diet, and oral hygiene helps minimize complications and promotes predictable healing. Patients are given guidance on safe pain management and steps to protect blood clot formation at surgical sites.
Follow-up visits allow the clinician to monitor healing, remove sutures if needed, and assess integration of grafts or implants. Most daily activities resume within a few days to a couple of weeks, although more extensive reconstruction may require a longer recovery period. Patients are advised to contact the office promptly for signs such as persistent bleeding, fever, or increasing pain.
Bone grafting and sinus lift procedures rebuild or augment deficient jawbone to provide a stable foundation for dental implants. Grafts may use the patient’s own bone, donor bone, or synthetic materials and are shaped to restore ridge height and width where implants will be placed. Sinus lifts elevate the sinus membrane and add bone to the upper jaw when the sinus anatomy limits implant depth.
Healing time varies with the extent of augmentation but typically involves a period of bone maturation before implant placement can proceed. The clinician monitors graft integration with clinical exams and imaging to determine the optimal timing for restoration. Proper planning and meticulous surgical technique improve the likelihood of predictable, long-term success.
Surgical endodontics, such as apicoectomy, is indicated when conventional root canal therapy cannot resolve persistent infection at the root tip. These procedures remove the infected tissue and seal the root end to preserve the natural tooth when retreatment alone is unlikely to succeed. Microsurgical techniques and magnification improve visualization and precision during these targeted interventions.
Candidates for surgical endodontic treatment undergo thorough evaluation including imaging to map root anatomy and adjacent structures. Recovery is generally quick, and follow-up imaging confirms healing over time. When successful, these procedures maintain tooth function and avoid extraction in many cases.
Facial trauma and dental emergencies demand prompt assessment to stabilize the patient, control bleeding, and protect the airway when necessary. The initial response focuses on pain control, infection prevention, and short-term stabilization of injured teeth or bone fragments. Advanced imaging and surgical planning follow once the patient is stable to guide definitive repair.
Treatment may include repositioning fractures, fixation of bony segments, repair of soft tissue injuries, or extraction of non-restorable teeth. Coordination with medical or surgical specialists is arranged for complex injuries affecting facial structures or when systemic concerns exist. Timely surgical intervention reduces the risk of long-term functional and aesthetic problems.
Surgical options for obstructive sleep apnea and airway obstruction are considered when conservative therapies, such as oral appliances or positive airway pressure, do not provide adequate relief. Surgical evaluation identifies anatomical contributors to obstruction and may recommend procedures that expand the airway or reposition soft tissues. Recommendations are individualized and often involve collaboration with sleep medicine or ENT specialists.
The goal of surgical management is to improve airway patency, reduce daytime sleepiness, and lower health risks associated with untreated sleep apnea. Preoperative sleep testing and imaging inform the treatment plan and expected outcomes. Patients receive counseling on risks, recovery, and how surgery integrates with non-surgical therapies.
Modern oral surgery relies on imaging and digital planning tools that enhance safety and predictability, such as cone-beam computed tomography and virtual surgical simulation. These technologies help clinicians visualize bone volume, nerve pathways, and sinus anatomy, enabling precise implant placement and avoidance of critical structures. Guided surgical templates translate digital planning into accurate intraoperative execution.
Magnification, microsurgical instruments, and minimally invasive techniques reduce tissue trauma and speed healing, while monitored sedation protocols support patient comfort during procedures. The surgical team follows strict infection control and monitoring standards to maintain safety throughout treatment. Ballston Dental Center combines these technologies with personalized planning to achieve reliable functional and aesthetic outcomes.
We are here to help you take the next step toward a healthier smile.
Whether you have questions about our services, insurance, or scheduling your first visit, our team is ready to assist you.
We welcome new and returning patients and are happy to help you find a time that fits your schedule. Reach out to our office today to schedule an appointment or learn more about how we can support your oral health. We look forward to welcoming you to our practice.