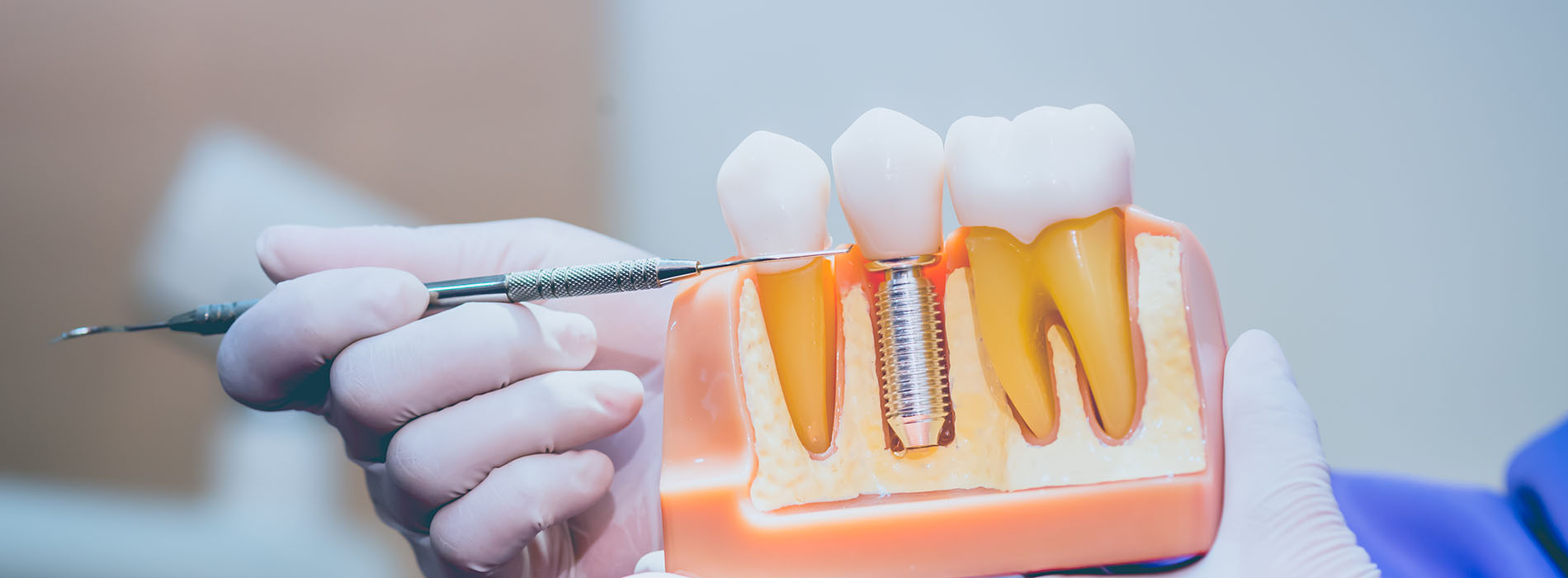
When a dental implant is placed, the visible portion that restores chewing, speech, and appearance is called the implant restoration. Unlike removable dentures or traditional bridges that rely on adjacent teeth or soft tissue for support, implant restorations attach to a titanium or zirconia implant anchored in the jawbone. This integration creates a stable foundation that reproduces the feel and function of a natural tooth more closely than many other replacement options.
Implant restorations come in several forms: a single crown to replace one missing tooth, a fixed bridge supported by multiple implants, or attachments that stabilize a removable denture. The restoration itself can be screw-retained or cement-retained, each approach offering distinct advantages in terms of retrievability, maintenance, and esthetics. Choosing the right type depends on the location of the missing teeth, the condition of surrounding tissue, and long-term maintenance plans.
Understanding the distinction between the implant (the part in the bone) and the restoration (the visible replacement) helps patients set realistic expectations. The implant provides structural support, while the restoration restores shape, color, and bite. When planned and executed properly, implant restorations can preserve adjacent teeth, maintain jawbone volume, and provide predictable function for many years.
Successful implant restorations start with careful planning. During the initial consultation, the dentist evaluates oral health, takes dental imaging, and discusses goals and medical history. Digital scans or conventional impressions capture the exact shape of the mouth, which allows the clinical team and dental laboratory to design restorations that fit the implant position and the patient’s bite precisely. The planning stage also determines whether additional preparatory work — such as bone grafting or soft tissue augmentation — is necessary before restoration placement.
After the implant has been placed and given time to integrate with the bone, the restorative phase begins. The clinician will attach an abutment — a small connector — to the implant and take detailed records to match tooth color, shape, and contours. Some patients receive a provisional restoration during this stage to protect the site and allow the team to refine the final design based on function and esthetics. The final restoration is fabricated from durable dental materials and adjusted chairside for a comfortable bite and natural appearance.
The timeline varies from case to case. Some implants are ready for restoration after a few months of healing, while others may require additional procedures that extend the schedule. Throughout the process, communication between the dentist, the dental laboratory, and the patient ensures the final result balances durability with a lifelike look that complements the patient’s smile.
Modern implant restorations use a range of materials chosen for strength, wear resistance, and esthetic qualities. All-ceramic restorations, such as those made from zirconia or lithium disilicate, are popular for their translucency and ability to mimic natural tooth enamel. Porcelain-fused-to-metal (PFM) remains a viable option in areas where strength is paramount. The material selected depends on the tooth’s position, the amount of bite force it will endure, and the patient’s esthetic priorities.
Design decisions also factor into the long-term success of restorations. Screw-retained restorations provide easier retrievability for adjustments or repairs without disturbing the crown, while cement-retained options can offer slightly improved esthetics in certain situations. The emergence profile — how the restoration meets the gumline — is shaped to support healthy soft tissue and create a seamless transition between restoration and natural tooth structure. Precision engineering and color-matching are both essential to delivering results that look and feel integrated.
Beyond material selection, occlusal design (how the teeth meet during chewing) is critical. A restoration must distribute bite forces evenly to protect the implant and surrounding bone. Careful adjustments during delivery reduce the risk of overload and contribute to a more comfortable, long-lasting restoration.
Most adults with missing teeth are potential candidates for implant restorations, but candidacy depends on oral and overall health. Healthy gums and sufficient jawbone are important for implant stability; however, many patients who initially lack adequate bone can qualify after bone grafting or regenerative procedures. The dentist reviews medical history for conditions that may affect healing, such as uncontrolled diabetes or tobacco use, and works with patients to optimize health prior to treatment.
Preparation can include periodontal treatment to resolve gum disease, tooth extractions, or site augmentation to create a stable foundation for the implant. These preparatory steps protect the long-term prognosis of the restoration and help create predictable esthetic results. The treatment plan is individualized — some patients follow a straightforward timeline, while others require staged procedures to ensure the best outcome.
During each appointment, the team explains the steps, expected healing times, and what patients can expect in terms of comfort and function. Minimally invasive techniques and appropriate anesthesia or sedation options are used to promote patient comfort. Clear post-operative instructions and follow-up visits are an integral part of the process to monitor healing and readiness for the final restoration.
Once a restoration is in place, routine home care and professional maintenance are the keys to longevity. Daily brushing and flossing adapted for implants — including interdental brushes or floss designed for implant-supported teeth — remove plaque and help prevent inflammation around the implant. Patients are advised to maintain consistent oral hygiene habits, as peri-implant mucositis and peri-implantitis can undermine even well-constructed restorations.
Regular dental visits allow the clinical team to check fit, occlusion, and tissue health around the restoration. Periodic professional cleanings and examinations catch early changes before they evolve into complications. In some cases, components such as screws or abutments may need tightening or replacement over time; having a restoration that is accessible and serviceable simplifies those interventions and preserves function.
Patients should also be mindful of habits that can stress restorations, such as chewing on hard objects or chronic grinding. When bruxism is present, a protective nightguard can reduce wear and protect both natural teeth and implant restorations. With consistent care and timely attention to any concerns, implant restorations can provide stable function and esthetics for many years.
At Ballston Dental Center, our approach to implant restorations combines modern materials, careful planning, and patient-centered communication to restore both function and confidence in the smile. If you are considering implant-supported crowns, bridges, or denture attachments, we can help you understand the options and create a personalized plan that aligns with your goals. Contact us to learn more or to schedule a consultation — we’re happy to discuss how implant restorations may fit into your long-term oral health strategy.

An implant restoration is the visible replacement that attaches to a dental implant to restore chewing, speech and appearance. It is the prosthetic part — such as a crown, bridge or denture attachment — that connects to a titanium or zirconia implant anchored in the jawbone. Because the restoration is fixed or securely retained to the implant, it reproduces the form and function of a natural tooth more closely than many removable options.
Understanding the role of the restoration helps patients set realistic expectations: the implant provides structural support while the restoration restores shape, color and occlusal function. When planned with attention to anatomy and bite forces, implant restorations can preserve adjacent teeth and help maintain jawbone volume. Long-term success depends on precise fit, appropriate materials and ongoing maintenance.
The implant is the part placed into the jawbone and serves as the artificial root, while the restoration is the visible tooth-shaped prosthesis attached to that implant. The implant achieves stability through osseointegration, which provides the foundation for the restoration to support chewing and speech. The restoration is designed to replicate tooth anatomy, color and occlusion so it blends with surrounding teeth and restores function.
Separating these concepts is important for treatment planning and maintenance because the implant and the restoration can require different types of care or interventions. For example, the implant may be evaluated radiographically for bone support, while the restoration is assessed for fit, wear and esthetics. Recognizing the distinction also clarifies why some repairs or adjustments can be performed without disturbing the implant itself.
Common implant restorations include single crowns for individual tooth replacement, fixed bridges supported by multiple implants, and attachments that stabilize removable dentures. Single crowns restore one missing tooth, while implant-supported bridges replace several adjacent teeth without relying on neighboring natural teeth for support. Implant-retained overdentures use attachments or bars to secure a denture and improve retention and function compared with conventional removable prostheses.
Restorations can be designed as screw-retained or cement-retained, each offering specific advantages in retrievability and esthetics. Screw-retained designs allow easier access for maintenance or repairs, while cement-retained options can provide a streamlined emergence profile in select cases. The choice depends on implant position, soft tissue considerations and the long-term maintenance strategy discussed during planning.
Implant restorations are made from materials chosen for strength, wear resistance and esthetic qualities, including zirconia, lithium disilicate and porcelain fused to metal. All-ceramic materials like zirconia and lithium disilicate are popular for their translucency and lifelike appearance, making them a good match for front teeth. Porcelain-fused-to-metal remains a reliable option where high occlusal load or limited space requires added strength.
Material choice is driven by tooth position, bite forces and esthetic priorities, as well as the restoration's design and connector requirements. Laboratory precision and color-matching protocols further influence the final appearance and function. The clinician explains trade-offs so patients understand durability, maintenance and expected wear characteristics for the selected material.
The restoration workflow begins with a consultation that includes an oral exam, medical history review and diagnostic imaging to assess bone, soft tissue and adjacent teeth. Digital scans or conventional impressions capture the mouth's shape for laboratory planning, and the team determines whether preparatory procedures such as extractions, bone grafting or soft tissue augmentation are needed. Treatment sequencing is individualized to ensure an optimal foundation before the restorative phase begins.
After implant placement and a healing period to allow integration, the clinician attaches an abutment and records shade and contours for the final restoration, sometimes placing a provisional to refine esthetics and function. The laboratory fabricates the definitive restoration, which is adjusted chairside for occlusion and comfort before final delivery. Follow-up visits confirm tissue health and occlusal stability to support long-term success.
Most adults with one or more missing teeth are potential candidates for implant restorations, but candidacy depends on oral and overall health. Key factors include healthy gum tissue, sufficient jawbone volume or a plan for augmentation, and general medical conditions that support predictable healing. The dentist evaluates medication use, systemic conditions such as diabetes and habits like tobacco use to identify factors that may affect outcomes and to develop an appropriate care plan.
When patients initially lack adequate bone or soft tissue, staged procedures such as bone grafting or connective tissue grafts can often create a suitable site for implants. Periodontal health is addressed before restorative work to reduce the risk of complications. A thorough evaluation allows a tailored approach that balances functional needs, esthetic goals and long-term prognosis.
Preparation begins with a comprehensive evaluation that may include periodontal therapy, extractions or site development to create a stable foundation for the implant and eventual restoration. The clinician reviews medical history and coordinates with other health care providers as needed to optimize conditions for healing. Patients are advised on oral hygiene measures, smoking cessation and any preoperative instructions for the planned procedures.
During treatment planning, the team explains expected healing timelines, potential staging of procedures and available anesthesia or sedation options to promote comfort. Clear post-operative instructions are provided to support recovery and reduce the risk of complications. Regular follow-up visits are scheduled to monitor healing and to determine the appropriate timing for restorative work.
Routine home care and professional maintenance are essential to protect implant restorations over time. Daily brushing and interdental cleaning around implants removes plaque and helps prevent peri-implant mucositis and peri-implantitis, conditions that can jeopardize even well-made restorations. Patients should use tools recommended by their clinician, such as interdental brushes or implant-specific floss, and maintain consistent oral hygiene habits.
Regular dental visits allow the clinical team to check restoration fit, occlusion and the health of surrounding tissues, and to perform professional cleanings that reach beneath the gumline if needed. Some components, such as screws or abutments, may require occasional adjustment or replacement to maintain function. Early detection and timely management of changes help preserve both the restoration and supporting structures.
Complications associated with implant restorations can include soft tissue inflammation, component loosening, restoration fracture or excessive wear, and in rare cases peri-implant bone loss. Many issues are identified during routine recall visits and can be managed with noninvasive measures such as improved hygiene coaching, professional debridement or tightening and replacement of restorative components. More advanced problems may require regenerative procedures or restoration remakes when indicated.
Prevention and early intervention are central to managing risks, which is why appropriate material selection, occlusal design and regular monitoring are emphasized during planning and follow-up. Patients are encouraged to report discomfort, mobility or changes in fit promptly so the team can evaluate and intervene. A predictable maintenance protocol reduces the likelihood of escalation and supports long-term success.
Our approach emphasizes careful planning, precise restorative design and clear communication so patients understand each stage of treatment and the expected outcomes. We use diagnostic imaging and digital records to coordinate treatment between the surgical and restorative phases, and we select materials and retention methods that balance esthetics, function and serviceability. The team discusses personalized timelines and any preparatory steps needed to create a healthy foundation for the restoration.
During delivery and follow-up, we focus on occlusal harmony and soft tissue support to promote comfort and long-term stability, and we provide practical guidance for home care and maintenance. Patients receive routine monitoring to catch early changes and simplify any required interventions. This collaborative, patient-centered process helps restore function and confidence while protecting oral health for years to come.
We are here to help you take the next step toward a healthier smile.
Whether you have questions about our services, insurance, or scheduling your first visit, our team is ready to assist you.
We welcome new and returning patients and are happy to help you find a time that fits your schedule. Reach out to our office today to schedule an appointment or learn more about how we can support your oral health. We look forward to welcoming you to our practice.