Losing one or more teeth affects more than just the way your smile looks — it changes how you eat, speak, and feel about yourself. Advances in modern dentistry offer a reliable path to restore both function and appearance, and dental implants lead that progress. At Ballston Dental Center, we help patients explore implant solutions that are designed to perform like natural teeth and last for many years with proper care.

Rather than relying on removable prosthetics or altering neighboring teeth to fill a gap, implants replace a tooth’s root with a biocompatible post that supports a crown, bridge, or denture. This root-level restoration stabilizes chewing forces, preserves jawbone health, and creates a base for restorations that look, feel, and function very much like natural teeth.
A dental implant is engineered to integrate with the bone that once held your tooth root. That integration — called osseointegration — provides a solid foundation for replacement teeth and recreates the mechanical behavior of a real tooth. The visible portion (a crown or prosthesis) is custom-matched to the surrounding teeth so the result is both comfortable and visually harmonious.
Implants support a wide range of restorations: a single crown to replace one missing tooth, bridges that span multiple teeth without altering adjacent healthy teeth, and full-arch prostheses that restore an entire upper or lower jaw. For many people, implants eliminate common denture concerns such as movement, slippage, and difficulty eating certain foods.
Because implants act like true tooth roots, they also help preserve the jawbone. That biological benefit reduces the gradual bone loss that usually follows tooth extraction and supports natural facial contours over time.
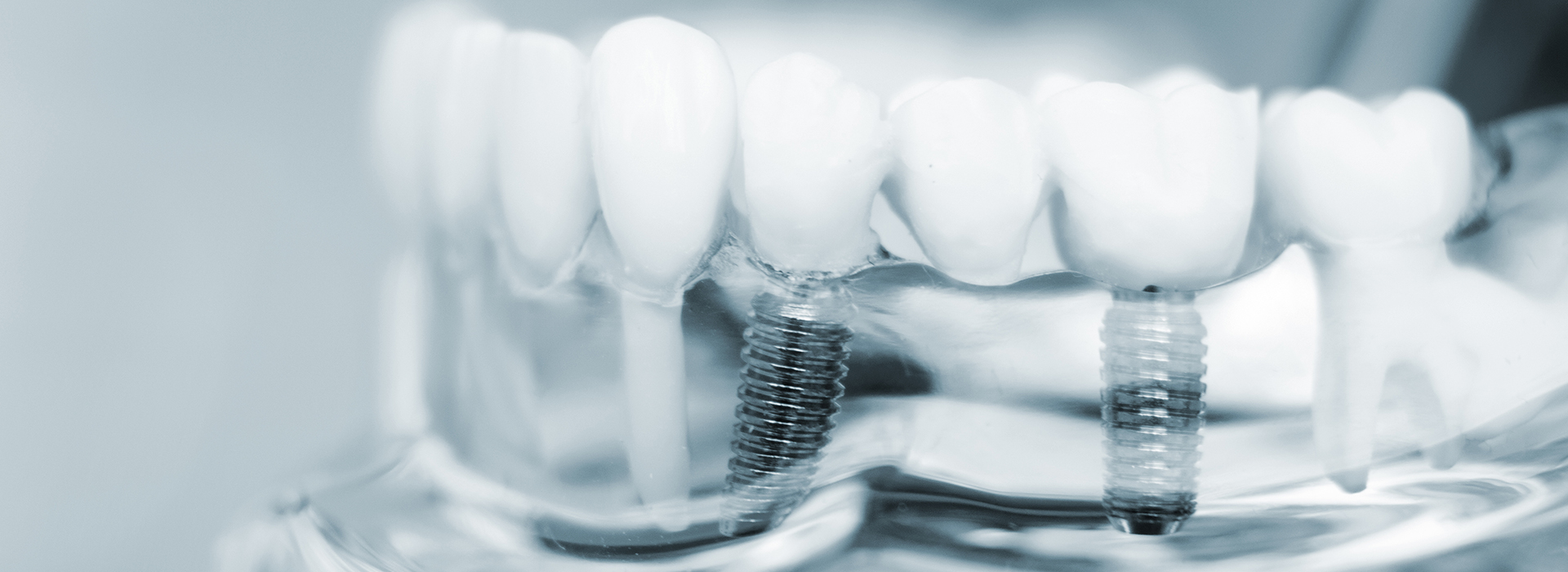
At its core, a dental implant consists of three parts: the implant post (usually titanium or a titanium alloy), an abutment that connects the post to the replacement tooth, and the prosthetic tooth itself. The post is surgically placed into the jawbone; over the following months the surrounding bone grows around the post, stabilizing it firmly in place.
Because the implant becomes anchored to bone rather than resting on gum tissue, it transfers chewing forces through the jaw in a way that promotes healthy bone maintenance. This is one reason implants are considered the most complete long-term solution for missing teeth.
The treatment timeline varies: some patients receive a temporary prosthesis at the time of implant placement, while others wait for full bone healing before the final restoration is attached. Your dental team will recommend the option that best balances safety, function, and esthetic outcome for your unique situation.
Beyond cosmetic improvements, implants deliver measurable oral-health benefits. By replacing the tooth root, implants maintain the stimulation that bone requires to stay healthy. This helps prevent the bone shrinkage and facial changes that sometimes follow long-term tooth loss.
From a day-to-day perspective, implants restore chewing efficiency and speech clarity. Patients commonly report being able to enjoy a greater variety of foods and feeling more comfortable speaking and smiling without worrying about movement or adhesives that are sometimes necessary with traditional dentures.
Longevity is another key advantage. With precision placement and routine dental care, implants can remain functional for many years. Because implants are made from materials that do not decay, they do not develop cavities; instead, long-term success depends on periodontal health and regular maintenance.
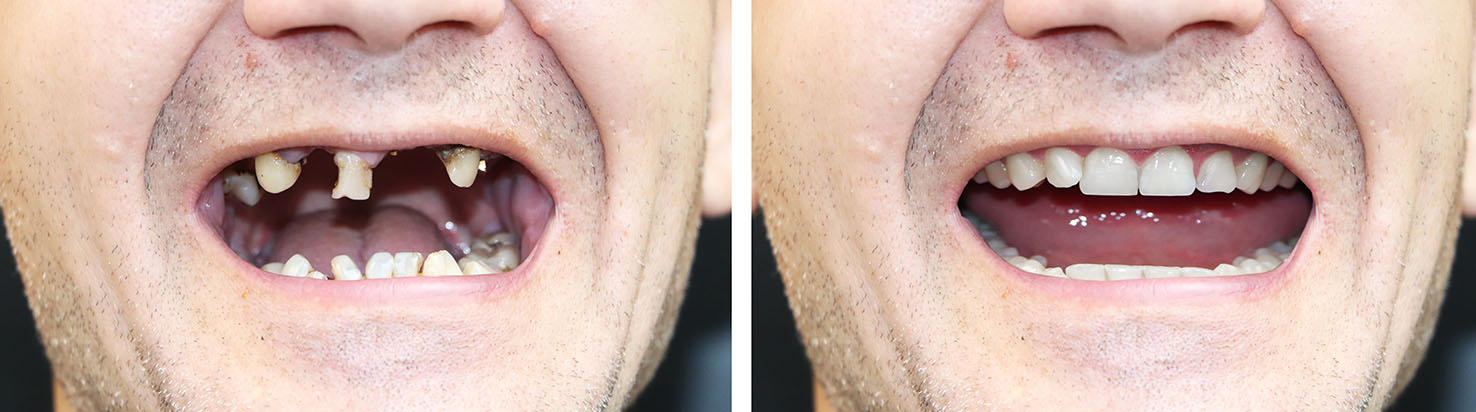
Dental implants are a flexible solution. The right approach depends on how many teeth are missing, the quality and quantity of available bone, and the patient’s goals for comfort, appearance, and function. Your clinician will recommend a customized plan that addresses both immediate needs and long-term oral health.
Single-tooth implants restore one missing tooth without disturbing adjacent teeth. For gaps involving several teeth, implant-supported bridges provide a strong, conservative option that preserves the integrity of surrounding dentition. For patients missing an entire arch, a fixed full-arch restoration or implant-retained denture can reestablish a confident, natural-feeling smile.
Each option balances predictability and patient preference. Modern implant dentistry also offers choices in materials and prosthetic design, so restorations can be optimized for esthetics, strength, and ease of hygiene.
Determining whether implants are the best choice starts with a comprehensive evaluation. Your dentist will review your medical and dental history, assess gum and bone health, and use imaging to map the jaw. This diagnostic work identifies the ideal locations for implants and helps anticipate any preparatory steps.
Some patients require additional procedures before implant placement, such as bone grafting to rebuild lost volume or tooth extractions to clear space. These preparatory treatments are common and routinely performed to create a stable foundation for long-term implant success.
We design each treatment plan to reflect a patient’s overall health, lifestyle, and goals. Clear communication about timelines, healing expectations, and maintenance is a core part of that planning process so patients feel informed and prepared at every stage.
Implant placement is typically performed as an outpatient procedure using local anesthesia, and options for sedation are available when appropriate. The post-operative period usually involves mild to moderate discomfort and swelling that subsides over several days. Care instructions help manage discomfort and support healing.
Osseointegration — the process of bone bonding to the implant — takes several months in most cases. During that time, temporary restorations can maintain esthetics while the implant becomes secure. Once healing is complete, the final prosthetic is attached and refined to ensure proper bite and appearance.
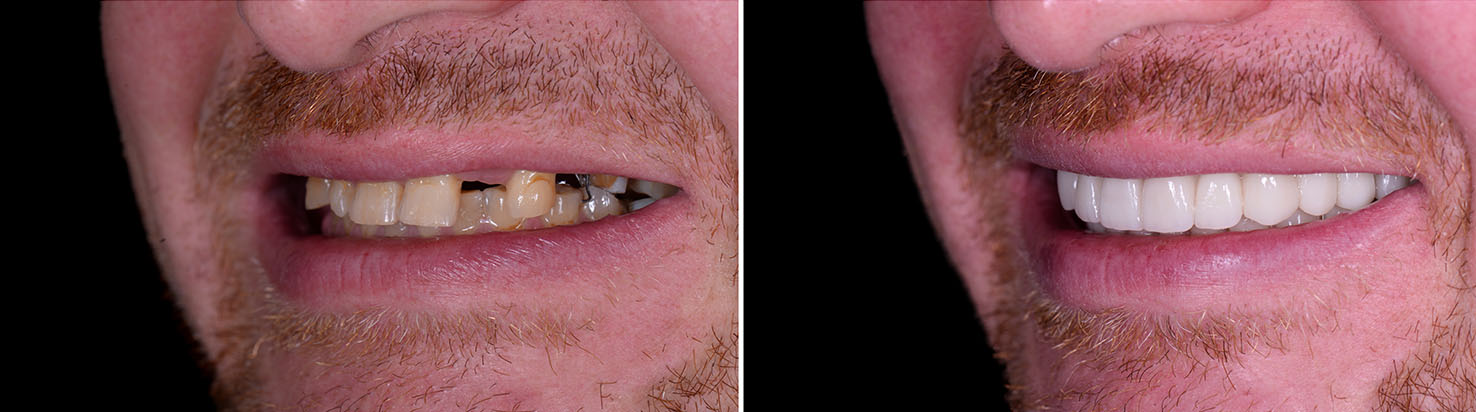
Implant success depends on having enough healthy bone to stabilize the post. If bone has been lost due to periodontal disease, injury, or the passage of time after tooth loss, a bone graft can rebuild the foundation needed for implantation. Grafting materials and techniques are varied and chosen to match the specific clinical requirement.
Adding bone where it’s needed not only makes implant placement possible, it improves long-term outcomes by creating better support for chewing forces and helping maintain facial form.
Choosing dental implants is a multi-step process that begins with a careful evaluation and concludes with a restoration that you care for as you would natural teeth. Success relies on precise treatment planning, skilled surgical placement, and a commitment to oral hygiene and routine dental visits.
At our practice, we emphasize patient education and collaboration: you’ll receive clear guidance about what to expect before, during, and after treatment, including recovery milestones and daily care tips for your new restoration.
Let Ballston Dental Center help you explore whether implants are the right choice for restoring your smile. If you’d like to learn more about implant options, scheduling, or the evaluation process, please contact us for additional information and to arrange a consultation.

If you've lost a tooth due to injury, decay, gum disease, or any other reason, we recommend dental implants to replace missing teeth. Dental implants come the closest to replicating the look, feel, and function of your natural teeth.
Dental implants are placed into the jawbone and mirror the same function as the root of a tooth. The procedure for dental implants is usually performed while a patient is sedated. Patients who undergo IV sedation must have an empty stomach and transportation home following the procedure. Most sedation patients will have little to no memory of the procedure occurring.
Generally, dental implants are made out of a biocompatible metal such as titanium. Biocompatible metals are also used for other common bone implants (such as shoulder, hip, and knee replacements). The visible portion of the implant is usually made out of porcelain and is custom-made to match your existing teeth.
Dental implants are designed to fuse to the bone, which makes them become permanent fixtures. Typically speaking, the success rate is nearly 100%. There are few cases in which the implant will not fuse as intended and must be removed. If this happens to occur, the procedure can be attempted again a few months later.
Dental implants are not usually covered by dental insurance, but may be covered under a patient's medical insurance. Our office and your insurance company can discuss coverage options with you based on your individual case and treatment plan.
It's easy... just take care of an implant as if it's a natural tooth! This involves regular brushing, flossing, and dental checkups. If you have any concerns about your implant, contact us immediately.
Dental implants are artificial tooth roots that are surgically placed into the jaw to support replacement teeth. They are typically made from biocompatible materials that integrate with bone and provide a stable foundation for crowns, bridges, or dentures. Because implants restore the root as well as the visible tooth, they recreate much of the natural function and feel of a real tooth.
An implant restoration consists of three main components: the implant post, an abutment that connects the post to the prosthesis, and the crown or denture that serves as the visible tooth. Once the post bonds with surrounding bone through osseointegration, the restoration is attached and adjusted for bite and appearance. This root-level approach helps distribute chewing forces and supports long-term oral health.
Good candidates for dental implants are patients who are in overall good health, have adequate jawbone to support an implant, and are committed to routine oral care. A comprehensive evaluation including medical history, periodontal assessment, and imaging will determine whether an implant is appropriate and whether preparatory procedures are needed. Certain conditions like uncontrolled diabetes or heavy tobacco use can affect healing, so these factors are discussed during treatment planning.
Older age alone does not preclude implant treatment; many healthy seniors are excellent candidates. If bone volume is limited, procedures such as bone grafting can create the necessary support for an implant. Your dentist will explain the risks and expected outcomes so you can make an informed decision based on your health and goals.
The implant process begins with a detailed consultation and diagnostic imaging to map the jaw and plan implant placement. Implant surgery is performed as an outpatient procedure using local anesthesia and, when appropriate, sedation to ensure patient comfort. After placement, a healing period allows bone to grow around the implant, a process that typically takes several months depending on individual healing factors.
Patients may receive a temporary prosthesis during the healing phase to preserve esthetics and function, or the final restoration may be placed after osseointegration is complete. The overall timeline varies with the complexity of the case, any required preparatory treatments, and the chosen restoration. Your dental team will outline a clear schedule and milestones so you know what to expect at each stage.
Implant restorations are highly adaptable and can replace a single tooth, several teeth, or an entire arch. Options include single-tooth crowns, implant-supported bridges that span multiple missing teeth without altering adjacent healthy teeth, fixed full-arch prostheses supported by several implants, and implant-retained overdentures that snap into place for improved retention. Each restoration type is selected based on the number of missing teeth, bone quality, and the patient’s preferences for permanence and maintenance.
Materials and prosthetic designs can be customized to balance esthetics, strength, and hygiene access. For full-arch rehabilitation, clinicians often recommend a fixed prosthesis when stability and long-term function are priorities, while overdentures may suit patients who prefer a removable option with enhanced retention. Your dentist will review the benefits and practical considerations of each approach for your situation.
A bone graft is recommended when the jaw lacks sufficient volume or density to stabilize an implant post. Bone loss can occur after tooth extraction, periodontal disease, or injury, and inadequate bone increases the risk of implant failure unless the foundation is rebuilt. Grafting restores bone height and width, creating a stable environment for osseointegration and improving long-term outcomes.
Grafting techniques and materials vary from using the patient’s own bone to synthetic or donor graft materials chosen to match the clinical need. Healing after a graft can take several months before an implant is placed, though in some cases grafting and implant placement are performed in the same visit. Your dental team will recommend the appropriate grafting approach and timeline based on diagnostic imaging and treatment goals.
Implant placement is generally an outpatient procedure performed under local anesthesia, and sedation options are available for patient comfort when needed. Immediately after surgery patients can expect some swelling, mild to moderate discomfort, and manageable bleeding for the first 24 to 48 hours. Clinicians provide clear post-operative instructions including pain management strategies, wound care, and activity restrictions to support healing.
Follow-up visits monitor soft tissue healing and the progress of osseointegration over the following weeks and months. Most patients return to normal light activities within a few days and resume a regular diet as healing allows and as advised by the dentist. Any unusual or persistent symptoms should be reported promptly so the team can evaluate and address them.
Long-term success of dental implants depends on excellent daily oral hygiene and regular professional care. Patients should brush twice daily, floss or use interdental cleaners around implant restorations, and maintain routine dental visits for periodontal evaluation and professional cleaning. Good gum health is critical because implants do not decay, but the surrounding tissues can develop inflammation if plaque control is inadequate.
Prosthetic components also require periodic inspection and maintenance to ensure proper fit and function. Your dentist will advise on specific cleaning techniques for your restoration and recommend a recall schedule to monitor bone levels, soft tissue health, and the integrity of the prosthesis. Adhering to these recommendations helps maximize implant longevity.
As with any surgical procedure, dental implants carry some risks, including infection, implant failure, nerve irritation, and sinus complications for upper jaw placements. Early failures are often related to infection or inadequate healing, while late failures can result from biomechanical overload or progressive bone loss around the implant. Careful planning, sterile surgical technique, and good oral hygiene reduce these risks significantly.
Some patients may experience temporary numbness or altered sensation if nearby nerves are affected, and implants placed in the upper jaw require precise evaluation to avoid the sinus cavity. Your dentist will review potential complications specific to your anatomy and health history and describe steps taken to mitigate those risks before you proceed.
Dental implants offer root-level support that helps preserve jawbone and maintain facial contours, which is an advantage over traditional dentures that rest on gum tissue. Unlike bridges that rely on adjacent teeth for support, implants can replace a missing tooth without altering neighboring healthy teeth. Many patients find that implants restore chewing efficiency and speech more closely to natural teeth than removable options.
That said, dentures and bridges remain appropriate solutions in certain clinical situations or when patient preferences favor those approaches. The choice among implants, bridges, and dentures depends on medical and dental health, anatomy, and the patient’s functional and esthetic goals. A careful discussion with your dentist will identify the most suitable option for your needs.
At Ballston Dental Center we begin implant care with a comprehensive evaluation that includes medical and dental history, periodontal assessment, and diagnostic imaging such as CBCT when indicated. This planning phase maps bone volume, identifies vital structures, and helps the team select implant size and position for optimal function and esthetics. Treatment plans are personalized to reflect each patient’s health, lifestyle, and restorative goals.
The practice emphasizes clear communication and collaborative care, explaining each step of the process, expected timelines, and post-operative instructions. We coordinate any necessary preparatory procedures, offer sedation options when appropriate, and provide ongoing follow-up to monitor healing and prosthetic performance. This systematic approach helps patients feel informed and confident throughout implant treatment.
We are here to help you take the next step toward a healthier smile.
Whether you have questions about our services, insurance, or scheduling your first visit, our team is ready to assist you.
We welcome new and returning patients and are happy to help you find a time that fits your schedule. Reach out to our office today to schedule an appointment or learn more about how we can support your oral health. We look forward to welcoming you to our practice.